Anne CC Lee, Lian Folger, Lauren Schaeffer, Pratik Panchal, Hannah Blencowe, Joy E Lawn
Nov 17, 2017 is World Prematurity Day. The authors publication on diagnostic accuracy in neonatal assessment was released today in Pediatrics.
 On World Prematurity Day, findings from a new study will be published in the journal Pediatrics.1 This systematic review examines the accuracy of different newborn assessments to determine gestational age and identify preterm babies.
On World Prematurity Day, findings from a new study will be published in the journal Pediatrics.1 This systematic review examines the accuracy of different newborn assessments to determine gestational age and identify preterm babies.
WHY THE EARLY IDENTIFICATION OF PRETERM BABIES IS IMPORTANT
Each year, 15 million babies are estimated to be born preterm (before 37 completed weeks gestation), with the vast majority born in low- and middle-income countries (LMICs).2 Preterm birth complications are the leading cause of under-5 child mortality globally3—accounting for 1 million neonatal deaths each year.4
Preterm babies are more likely to die in infancy or become ill with conditions that could be effectively treated if identified early, such as breathing problems, infections, or low body temperature. The early identification of preterm babies enables health workers to offer these babies special care, including better monitoring and the timely delivery of potentially life-saving interventions, such as continuous positive airway pressure or kangaroo mother care. Furthermore, accurate determination of gestational age is needed to identify growth-restricted infants, who also carry increased risk of mortality and morbidity in infancy and beyond.
In order to save lives of premature and growth-restricted infants in LMICs, these high-risk infants need to be accurately identified as early as possible and targeted for interventions.
THE CHALLENGE OF PREGNANCY DATING IN LMICs
In LMICs, pregnancy-dating is challenging and often unavailable. Ultrasound-dating in early pregnancy is the most accurate method currently available to determine gestational age, and is the standard of care in high-income countries. However, access to ultrasound is low for pregnant women in LMICs — in rural sub-Saharan Africa, for example, less than 7% of pregnant women have an ultrasound in pregnancy.5 Furthermore, many pregnant women do not attend antenatal care until late in their pregnancy, when traditional ultrasound is notably inaccurate for determining gestational age. The most common alternative to ultrasound pregnancy-dating is maternal recall of last menstrual period (LMP), but this method is often unavailable or unreliable in LMICs, particularly in populations with high rates of maternal illiteracy.5,6 Symphysis fundal height, or measuring the height of the mother’s baby bump during pregnancy, is another alternative for LMICs. However, symphysis fundal height is imprecise in estimating gestational age (with a margin of error of +/- 6 weeks), and is influenced by other factors, such as fetal growth.
NEWBORN ASSESSMENT FOR ESTIMATING GESTATIONAL AGE
When the dating of pregnancy is unknown, the newborn can be examined after birth for signs of development and maturity to estimate its gestational age. Clinical assessment of newborn maturity has been used as a proxy to estimate gestational age after birth in high-income settings when pregnancy dating is uncertain, and may include a combination of physical signs (e.g., texture of the skin, shape of the ears) and neurologic signs (e.g., resting muscle tone). Although newborn assessments have become less relevant in high-income settings, they are often the only tool available to estimate gestational age in low-resource settings.
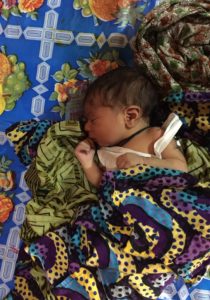 HOW ACCURATE ARE NEWBORN ASSESSMENTS FOR DETERMINING GESTATIONAL AGE?
HOW ACCURATE ARE NEWBORN ASSESSMENTS FOR DETERMINING GESTATIONAL AGE?
We conducted a systematic review to identify existing methods of assessing the newborn for gestational age and evaluated their accuracy compared to a reference “gold standard.”
We found 19 different newborn assessments that have been used to estimate gestational age, which include as few as 4 and as many as 23 signs of maturity. One of the most frequently used assessments is known as the Dubowitz score, which consists of 21 different physical and neurologic signs. Another commonly used assessment is the Ballard score, a shorter exam that comprises 12 physical and neurologic signs.
In our review of the literature, the Dubowitz score dated the majority of pregnancies within a window of +/- 2.6 weeks around a “gold standard” gestational age determined by ultrasound. The margin of error for the Ballard score was wider, dating most pregnancies within +/- 3.7 weeks of the “gold standard.” The Ballard score also tended to consistently overestimate gestational age by around half a week. Accordingly, the Ballard score could only identify 64% of babies born preterm, meaning that it would fail to identify one-third of preterm infants. In turn, those unidentified preterm babies may not be offered the extra care and monitoring that they need to survive and thrive.
Although more complex assessments are less feasible in LMICs, the simpler, and thus more feasible, assessments were found to be the least accurate, with wider margins of error. Several studies also found that newborn assessments were more biased and less accurate for estimating gestational age in the highest-risk babies (those born preterm and/or growth-restricted).
WHAT CAN BE DONE TO IMPROVE GESTATIONAL AGE MEASUREMENT IN LMICs?
Overall, these findings show that newborn assessments are currently not very accurate for identifying preterm babies. While more complex assessments (like the Dubowitz score) had better precision than simpler versions, they are more challenging to train and implement at large scale in low-resource settings.
Therefore, there is an urgent need to develop simpler and more accurate methods for estimating gestational age that are feasible to implement in LMICs.
Improving the accuracy of gestational age determination is a critical priority for newborn health and an emphasis of the Every Newborn Action Plan (http://www.who.int/maternal_child_adolescent/newborns/every-newborn/en/).
Priorities for improving gestational age measurement in LMICs include:
- Improving the coverage and accuracy of existing methods of pregnancy dating in LMICs
- Increasing coverage of ultrasound dating, preferably early in pregnancy
- Improving the accuracy of ultrasound assessment in later pregnancy
- Developing aids to improve the availability and accuracy of LMP recall (e.g. menstrual calendars)
- Increasing incentives to promote knowledge and reporting of gestational age by women and families
- Innovations to improve the accuracy of newborn assessment to determine gestational age
- Identifying new signs and combinations of newborn signs with improved validity, particularly in growth-restricted and preterm populations
- Assessing the feasibility of training and implementing existing, more complex scores in LMIC settings.
- Novel approaches to gestational age dating in the LMIC context
- Innovation for new tools, signs, testing, or technology that are feasible, valid and scalable in LMIC
The findings from this review are a call to action to the global public health community to augment efforts to improve the measurement of gestational age, in order to improve the survival and potential of preterm babies worldwide.
AUTHORS
Anne CC Lee, MD, MPH, FAAP is an Assistant Professor of Pediatrics at Harvard Medical School, practices clinical newborn medicine and directs Global Newborn Health Research in the Brigham and Women’s Hospital Department of Pediatric Newborn Medicine.
Lian Folger, BA is a Research Assistant in the Global Newborn Health Lab at Brigham and Women’s Hospital.
Lauren Schaeffer, MSc is the Project Manager of the Global Newborn Health Lab at Brigham and Women’s Hospital.
Hannah Blencowe, MBChB, MSc, MRCGP, PGCert, MedEd, MRCPCH is an assistant professor at the London School of Hygiene & Tropical Medicine, clinician, and perinatal epidemiologist.
Professor Joy Lawn, BMedSci, MB BS, MPH, PhD, MRCPCH, FMedSciis the Director of the MARCH Center at the London School of Hygiene and Tropical Medicine and a Senior Health Advisor to Save the Children.
Pratik Panchal, MD, MPH is a physician, a clinical research fellow at OpenBiome, and visiting scientist position at the Harvard T.H. Chan School of Public Health.
REFERENCES
- Lee AC, Panchal P, Folger L, et al. Diagnostic Accuracy of Neonatal Assessment for Gestational Age Determination: A systematic review. Pediatrics 2017; published online: 17 Nov 2017
- Blencowe H, Cousens S, Oestergaard MZ, et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet (London, England) 2012; 379(9832): 2162-72.
- Levels and Trends in Child Mortality: Report 2017. New York, NY: United Nation’s Children’s Fund, 2017.
- Liu L, Johnson HL, Cousens S, et al. Global, regional, and national causes of child mortality: an updated systematic analysis for 2010 with time trends since 2000. Lancet (London, England) 2012.
- Aliyu AD, Kurjak A, Wataganara T, et al. Ultrasound in Africa: what can really be done? J Perinat Med 2015; 44(22).
- Savitz DA, Terry JW, Jr., Dole N, Thorp JM, Jr., Siega-Riz AM, Herring AH. Comparison of pregnancy dating by last menstrual period, ultrasound scanning, and their combination. Am J Obstet Gynecol 2002; 187(6): 1660-6.